
Accessibility in Ambulatory Life Safety Plans

Introduction
Ensuring the safety and accessibility of ambulatory care facilities is paramount in providing a welcoming and inclusive environment for all individuals. One crucial aspect of this is the incorporation of accessibility needs into life safety plans. By accommodating these needs, ambulatory care facilities can ensure that individuals with disabilities or limited mobility can navigate the facility safely and independently.
Accessibility in ambulatory life safety plans involves implementing design elements and features that enable easy access, evacuation, and communication during emergencies. These plans should consider various factors such as accessible entrances, clear paths of travel, functional emergency systems, and appropriate signage.
But why is it so important to prioritize accessibility in life safety plans?
Imagine a scenario where an individual with a mobility impairment cannot evacuate a building swiftly during an emergency due to inaccessible exits or inadequate evacuation plans. Such situations can have devastating consequences, underscoring the critical need for comprehensive accessibility in life safety plans.
By integrating accessibility into life safety plans, ambulatory care facilities can not only meet legal requirements but also create an inclusive environment that promotes equal opportunities for all individuals. Moreover, considering accessibility needs during the planning phase can be more cost-effective than retrofitting inaccessible features later on.
When developing life safety plans, it is essential to consult relevant accessibility guidelines and standards, such as the Americans with Disabilities Act (ADA) and the International Code Council’s Accessible and Usable Buildings and Facilities (ICC A117.1). These documents provide detailed specifications for accessible design, ensuring compliance with legal requirements and promoting best practices.
But where can ambulatory care facilities turn for expert assistance in creating life safety plans that accommodate accessibility needs?
At Life Safety Express, we specialize in providing comprehensive guidance and solutions for ensuring accessibility in ambulatory life safety plans. With our deep understanding of accessibility regulations and industry best practices, we can assist you in creating plans that prioritize safety, inclusivity, and compliance.
By partnering with Life Safety Express, you can rest assured knowing that your ambulatory care facility will have a robust life safety plan that considers accessibility needs. Contact us today to learn more about how we can help you create a safer and more accessible environment for all.
- Understanding Ambulatory Life Safety Plans
- Legal Requirements for Accessibility in Healthcare Facilities
- Designing Accessible Routes and Exits
- Emergency Preparedness for Patients with Disabilities
- Best Practices for Implementing Accessibility Features
- Accessibility in Ambulatory Life Safety Plans: Frequently Asked Questions

Understanding Ambulatory Life Safety Plans
Ambulatory Life Safety Plans are a critical component in ensuring the safety and well-being of patients, staff, and visitors in healthcare facilities. These plans are designed to provide a comprehensive approach to fire safety, emergency response, and overall building security. A well-developed life safety plan takes into account the unique challenges that may arise in an ambulatory setting, where patients may have limited mobility or other disabilities that require special consideration.
At the core of an Ambulatory Life Safety Plan is the goal to protect lives and minimize potential injuries in the event of an emergency. This involves a detailed assessment of the facility’s layout, identifying potential hazards, and outlining clear evacuation procedures. It is essential for healthcare facilities to have a thorough understanding of the fire protection systems in place, including fire alarms, sprinklers, and smoke barriers.
Another key aspect of these plans is staff training and drills. Regular training ensures that all employees are familiar with the emergency procedures and can act quickly and efficiently if an incident occurs. Drills, on the other hand, provide an opportunity for staff to practice these procedures and identify any areas for improvement.
Furthermore, Ambulatory Life Safety Plans must be regularly reviewed and updated to reflect any changes in the facility’s design or operations. This ongoing process helps to maintain a high standard of safety and compliance with The Joint Commission (TJC) regulations.
Understanding Ambulatory Life Safety Plans is crucial for Executives, Administrators, Managers, and Safety Coordinators involved in healthcare facility management. These plans not only ensure compliance with TJC regulations but also provide a framework for creating a safe environment for everyone in the facility.
Legal Requirements for Accessibility in Healthcare Facilities
Healthcare facilities are subject to a myriad of legal requirements to ensure accessibility for all patients, including those with disabilities. These regulations are not just recommendations but are enforced by law, making compliance a critical aspect of healthcare administration. The Americans with Disabilities Act (ADA) sets forth standards that healthcare facilities must adhere to, ensuring that patients with disabilities have equal access to medical care.
Under the ADA, healthcare facilities are required to provide physical access to all areas where patient care is provided. This includes examination rooms, patient rooms, restrooms, and public areas such as waiting rooms and cafeterias. The law also requires that appropriate accommodations are made for effective communication with patients who have hearing, vision, or speech disabilities.
In addition to the ADA, healthcare facilities must also comply with the Architectural Barriers Act (ABA), which applies to buildings funded by the federal government. The ABA requires that facilities are designed and constructed to be accessible to individuals with disabilities. Furthermore, Section 504 of the Rehabilitation Act prohibits discrimination on the basis of disability in programs and activities that receive federal financial assistance.
Failure to comply with these legal requirements can result in significant consequences for healthcare facilities, including costly lawsuits, fines, and damage to reputation. It is imperative for healthcare executives and administrators to understand these legal obligations and ensure that their facilities meet or exceed the standards set forth by the ADA, ABA, and Section 504.
Compliance with these laws not only protects healthcare facilities from legal repercussions but also demonstrates a commitment to providing equitable care for all patients. By prioritizing accessibility, healthcare providers can enhance the patient experience, improve health outcomes, and uphold the ethical standards of the medical profession.
It is essential for healthcare facilities to conduct regular audits of their physical spaces and policies to ensure they are in line with current accessibility laws. When updates or renovations are necessary, they should be planned with accessibility in mind from the outset. By doing so, healthcare facilities can avoid the need for costly retrofits and ensure a welcoming environment for patients with disabilities from day one.
Designing Accessible Routes and Exits
When designing healthcare facilities, it is crucial to ensure that all routes and exits are accessible to individuals with disabilities. This includes not only patients but also staff and visitors who may require accommodations. The layout of corridors, doorways, ramps, and elevators must be carefully planned to allow for easy navigation and egress during an emergency.
Corridors should be wide enough to accommodate wheelchairs and other mobility aids, with handrails installed where necessary. Doorways need to be of a sufficient width and equipped with hardware that can be easily operated by individuals with limited dexterity. Ramps should have gentle slopes and non-slip surfaces, while elevators must be spacious and equipped with audible and visual signals for those with hearing or vision impairments.
In addition to physical accessibility, wayfinding is another critical aspect of design. Clear signage that includes Braille and high-contrast visuals can help guide individuals with visual impairments. Emergency exit maps should be displayed prominently and include information in accessible formats.
It is also important to consider the placement of emergency alarms and communication systems. These should be accessible to individuals of all heights and abilities, with visual alarms for those who are deaf or hard of hearing. In the event of an emergency, it is vital that everyone in the facility can receive alerts and instructions quickly and clearly.
Designing accessible routes and exits is not only a legal requirement but also a moral imperative. By taking into account the needs of all individuals, healthcare facilities can ensure that everyone has the ability to evacuate safely in an emergency. This proactive approach to design can save lives and prevent injuries, making it an essential component of any life safety plan.
Healthcare executives and safety coordinators should work closely with architects and builders to ensure that accessibility is integrated into the design from the beginning. Regular reviews and updates to the facility’s layout can also help identify any areas that may need improvement. By prioritizing accessibility in design, healthcare facilities can provide a safe and welcoming environment for all.
Emergency Preparedness for Patients with Disabilities
Emergency preparedness is a critical aspect of healthcare facility management, especially when it comes to ensuring the safety of patients with disabilities. It is essential to have a well-thought-out plan that addresses the unique needs of these individuals during an emergency situation. This includes having procedures in place for assisting patients with mobility, sensory, or cognitive impairments in the event of an evacuation.
One of the key components of emergency preparedness for patients with disabilities is staff training. Employees must be trained on how to assist patients with disabilities safely and efficiently. This includes understanding how to use evacuation chairs and other assistive devices, as well as knowing the location of accessible exits and safe areas. Staff should also be familiar with the various types of disabilities and the best ways to communicate with and assist those individuals.
In addition to staff training, healthcare facilities should conduct regular emergency drills that include scenarios involving patients with disabilities. These drills provide an opportunity to practice evacuation procedures and identify any potential challenges or areas for improvement. It is important that these drills are conducted in a manner that is respectful and sensitive to the needs of patients with disabilities.
Another important aspect of emergency preparedness is having the necessary equipment on hand. This includes having a sufficient number of evacuation chairs, wheelchairs, and other mobility aids readily available. Facilities should also have backup power systems in place to ensure that elevators and other critical equipment remain operational during a power outage.
Communication is also a vital part of emergency preparedness. Healthcare facilities should have systems in place to alert patients with hearing or vision impairments to an emergency. This may include visual alarm systems, tactile alerts, or other methods that ensure all patients receive timely and clear instructions.
By taking these steps, healthcare facilities can ensure that they are prepared to respond effectively to emergencies involving patients with disabilities. This not only helps to protect the safety and well-being of these individuals but also demonstrates a commitment to providing inclusive and equitable care.
It is the responsibility of healthcare executives, administrators, managers, and safety coordinators to ensure that their facilities are equipped and ready to handle emergencies involving patients with disabilities. By prioritizing emergency preparedness, healthcare facilities can provide peace of mind to patients and their families, knowing that their safety is taken seriously.
Best Practices for Implementing Accessibility Features
Implementing accessibility features in healthcare facilities is not just about meeting legal requirements; it’s about creating an inclusive environment that caters to the needs of all patients. To achieve this, there are several best practices that healthcare executives and safety coordinators should consider.
Firstly, involve individuals with disabilities in the planning process. By seeking input from those who will be directly impacted by accessibility features, facilities can ensure that their efforts are well-targeted and effective. This collaborative approach can also help identify potential issues that may not be immediately obvious to those without disabilities.
Secondly, invest in staff training. Employees should be well-versed in how to operate accessibility equipment and assist patients with disabilities. Training should be ongoing to keep staff updated on new technologies and best practices.
Thirdly, ensure that all accessibility features are well-maintained. Regular checks and maintenance are crucial to ensure that equipment such as lifts, ramps, and automatic doors are in good working order. A malfunctioning piece of equipment can quickly become a barrier rather than an aid.
Additionally, consider the use of technology to enhance accessibility. For example, implementing electronic health records that are accessible to patients with visual impairments can greatly improve their experience. Similarly, using apps or other digital tools can help patients with disabilities navigate the facility and access services more easily.
Lastly, create a culture of inclusivity within the facility. Encourage staff to be proactive in offering assistance and to treat all patients with respect and dignity. An inclusive culture not only benefits patients with disabilities but also contributes to a positive environment for all.
By following these best practices, healthcare facilities can go beyond mere compliance and become leaders in providing accessible care. This not only benefits patients with disabilities but also enhances the facility’s reputation and can lead to increased patient satisfaction and loyalty.
Implementing accessibility features is a multifaceted process that requires careful planning, training, maintenance, and cultural change. Healthcare executives and safety coordinators play a vital role in ensuring that these best practices are put into action, ultimately leading to a safer and more welcoming environment for all patients.
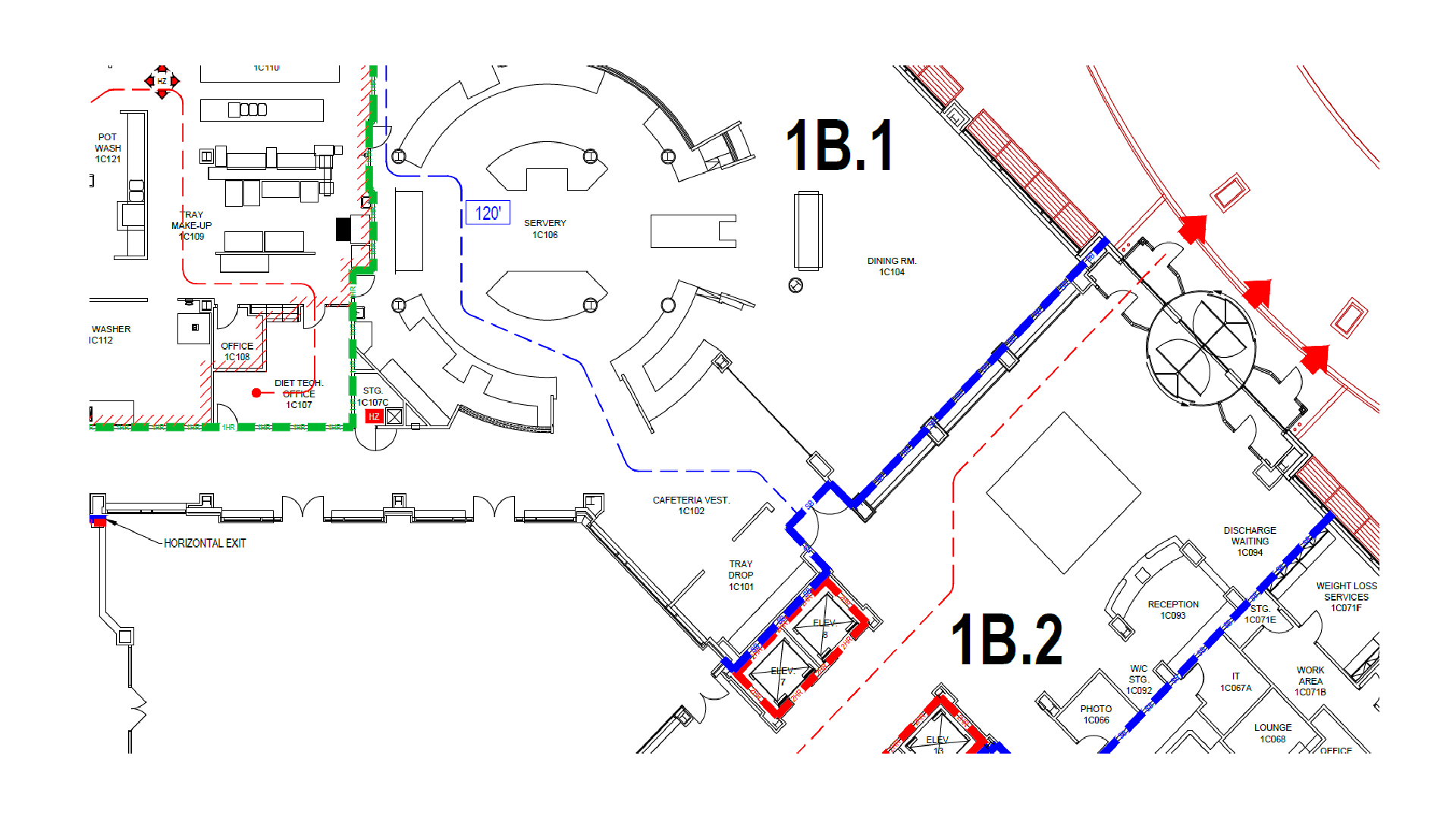
Accessibility in Ambulatory Life Safety Plans: Frequently Asked Questions
As you strive to ensure that your life safety drawings for ambulatory care facilities are accessible, you may come across various questions. We have compiled a list of frequently asked questions to provide you with the necessary guidance and insights. Read on to find answers to common queries related to accessibility in ambulatory life safety plans.
-
1. Why is it important to consider accessibility in ambulatory life safety plans?
Accessibility is crucial in ambulatory care facilities to ensure equal access and safety for all individuals, including those with disabilities or mobility challenges. By considering accessibility in your life safety plans, you can create an inclusive environment and comply with relevant regulations.
-
2. What are some key accessibility considerations when creating life safety drawings?
When creating life safety drawings, it’s important to consider elements such as accessible entrances, pathways, ramps, doorways, and elevators. You should also ensure that emergency evacuation routes are accessible and clearly marked, and that communication systems are inclusive for all individuals.
-
3. Are there specific accessibility codes or standards that need to be followed?
Yes, there are specific accessibility codes and standards that need to be followed when creating life safety plans for ambulatory care facilities. These may include the Americans with Disabilities Act (ADA), the International Building Code (IBC), and the National Fire Protection Association (NFPA) standards.
-
4. How can I ensure compliance with accessibility regulations?
To ensure compliance with accessibility regulations, it is advisable to consult with experts or professionals who specialize in accessibility design. They can provide guidance on interpreting and implementing the relevant codes and standards, and help you create accessible life safety plans.
-
5. What resources are available to assist in creating accessible life safety plans?
There are various resources available to assist you in creating accessible life safety plans. These may include accessibility guidelines and checklists provided by government agencies or organizations like the ADA, IBC, and NFPA. Additionally, consulting with accessibility experts or attending training workshops can provide valuable insights and support.
By considering these frequently asked questions, you can gain a better understanding of the importance of accessibility in ambulatory life safety plans. Remember, creating inclusive environments not only ensures compliance with regulations but also promotes equal access for all individuals.

