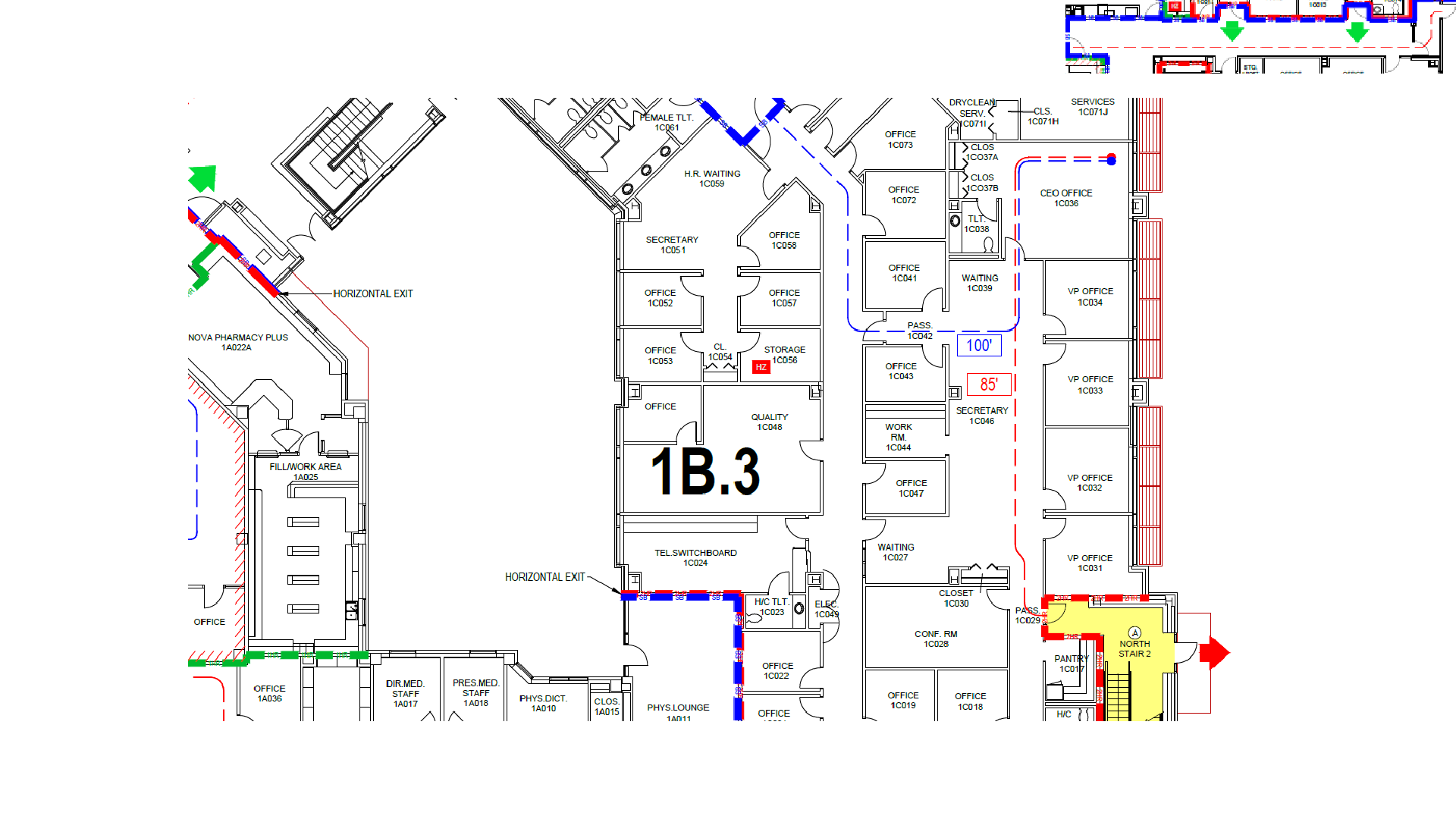
Building Code Compliance for Healthcare Facilities
[rev_slider alias=”LSE-magazine-content-slider1″][/rev_slider]

Ensuring Patient Safety: A Guide to Building Code Compliance for Healthcare Facilities
Understanding Building Code Compliance for Healthcare Facilities
When it comes to healthcare facilities, there is no room for compromise. The safety and well-being of patients, staff, and visitors are of utmost importance. That’s why understanding building codes and their implications for life safety in healthcare environments is crucial.
But what exactly are building codes? And how do they impact healthcare facilities?
Building codes are a set of regulations established by governing authorities to ensure the structural integrity, accessibility, and safety of buildings. In the case of healthcare facilities, compliance with these codes is not only required by law, but it also plays a vital role in protecting lives and minimizing risks.
So, what are the specific implications of building code compliance for healthcare facilities?
First and foremost, compliance with building codes ensures that healthcare facilities are designed and constructed to withstand natural disasters, such as earthquakes or fires. This means that the building’s structure, electrical systems, and fire protection measures are all carefully planned and implemented to provide the highest level of safety.
In addition to structural integrity, building code compliance also addresses accessibility for individuals with disabilities. This includes features such as ramps, elevators, and designated parking spaces, ensuring that everyone can access healthcare services without barriers.
But how can healthcare facilities ensure compliance with building codes?
Working with a knowledgeable and experienced partner is key. At Life Safety Express, we specialize in helping healthcare facilities navigate the complex world of building code compliance. Our team of experts understands the unique requirements of the healthcare industry and can provide practical solutions tailored to your facility’s needs.
Ready to ensure your healthcare facility meets all the necessary building code requirements?
Contact Life Safety Express today. Our team is here to guide you through the process, answering any questions you may have and providing the expertise needed to achieve compliance. Together, let’s create a safe and secure environment for all.
Table of Contents
- Overview of Healthcare Facility Regulatory Standards
- Design and Construction Requirements for Patient Safety
- Fire Safety and Emergency Preparedness in Healthcare Settings
- Accessibility and Accommodation Provisions in Medical Buildings
- Ongoing Compliance: Inspections, Maintenance, and Documentation
- Frequently Asked Questions about Building Code Compliance for Healthcare Facilities

Overview of Healthcare Facility Regulatory Standards
Healthcare facilities operate under a complex web of regulatory standards designed to ensure the highest level of patient care and safety. These regulations are multifaceted, covering everything from the physical structure of the building to the procedures that staff must follow. At the core of these standards is a commitment to creating an environment that supports the well-being and recovery of patients while also providing a safe workspace for healthcare professionals.
Central to these regulatory standards is The Joint Commission (TJC), an independent, not-for-profit organization that accredits and certifies nearly 21,000 health care organizations and programs in the United States. TJC accreditation is recognized nationwide as a symbol of quality that reflects an organization’s commitment to meeting certain performance standards. To maintain accreditation, facilities must undergo regular evaluations and demonstrate continuous compliance with TJC’s state-of-the-art standards.
These standards are developed in consultation with health care experts, providers, measurement experts, and patients. They are informed by scientific literature and expert consensus to help health care organizations measure, assess, and improve performance. The focus areas include patient rights and education, infection control, medication management, preventing medical errors, and ensuring a safe environment. The goal is not only to prevent avoidable harm but also to create a framework for organizational structure and management.
Moreover, healthcare facilities must also adhere to regulations set forth by federal agencies such as the Centers for Medicare & Medicaid Services (CMS) and the Occupational Safety and Health Administration (OSHA), as well as state and local health departments. These regulations encompass a broad range of concerns, including patient privacy laws under the Health Insurance Portability and Accountability Act (HIPAA), clinical laboratory improvement amendments (CLIA), and workplace safety protocols.
Compliance with these regulatory standards is not merely about following rules; it is about fostering a culture of safety and quality that permeates every aspect of healthcare delivery. It requires a proactive approach to risk management and a commitment to continuous improvement. For executives, administrators, managers, and safety coordinators, understanding these regulations is crucial for developing strategies that align with legal requirements and ethical responsibilities towards patients and staff alike.
By staying informed about the latest developments in healthcare regulations, leaders can ensure their facilities are not only compliant but also positioned to deliver the highest standard of care. This ongoing process of education and adaptation is essential in an industry where patient lives are at stake, and the landscape of healthcare is ever-evolving.
Design and Construction Requirements for Patient Safety
The design and construction of healthcare facilities are critical components in ensuring patient safety and must adhere to stringent standards. These standards are not only about aesthetics or functionality but are deeply rooted in the safety and well-being of patients, staff, and visitors. The physical environment must be conducive to healing, minimize risks of infection, and be resilient to emergencies.
From the initial planning stages, healthcare facilities must integrate patient safety into their architectural designs. This includes the selection of materials that are durable, easy to clean, and resistant to bacteria and other pathogens. Surfaces, flooring, and fixtures must be chosen with an eye towards infection control, a critical aspect in patient care areas.
Moreover, the layout of a healthcare facility is meticulously planned to optimize patient flow and minimize the potential for errors. For instance, clear signage and unobstructed corridors are essential for the safe and efficient movement of patients, particularly in emergency situations. The placement of nursing stations, medication dispensing areas, and support services are strategically positioned to enhance staff efficiency and patient access.
Another key aspect of design involves ensuring that all areas of the facility are adequately lit, ventilated, and temperature-controlled to promote a healing environment and prevent the spread of airborne illnesses. Special attention is given to patient rooms, treatment areas, and operating rooms where controlled environments are crucial for patient recovery and the prevention of post-operative infections.
Emergency systems such as backup power supplies, fire suppression systems, and medical gas systems are also integral to the design process. These systems must be reliable and meet all regulatory requirements to ensure they function effectively in the event of an outage or disaster.
Accessibility is another cornerstone of patient safety in healthcare facility design. This encompasses not only compliance with the Americans with Disabilities Act (ADA) but also creating an environment that accommodates patients with a wide range of physical abilities. Features such as ramps, handrails, wide doorways, and accessible bathroom facilities are essential for patient independence and safety.
In addition to these design elements, construction processes must also follow rigorous protocols to ensure that the work environment remains safe for existing patients and staff. This includes managing noise levels, dust control, and minimizing disruptions to ongoing healthcare services.
Ultimately, the design and construction of healthcare facilities are about creating spaces that support healing while protecting those who are vulnerable. It requires a meticulous approach that balances regulatory compliance with innovative design solutions that address the unique challenges of healthcare delivery. For those charged with overseeing these projects, it is a responsibility that demands a comprehensive understanding of both the needs of patients and the operational demands of healthcare providers.
Fire Safety and Emergency Preparedness in Healthcare Settings
Fire safety and emergency preparedness are paramount in healthcare settings, where the presence of vulnerable populations and complex equipment can create unique challenges. Healthcare facilities must have comprehensive fire safety programs that include prevention, containment, evacuation, and firefighting strategies. These programs are designed to protect patients, staff, and visitors from the dangers of fire and smoke, as well as to ensure continuity of care during and after an emergency.
One of the critical components of fire safety is the installation and maintenance of fire detection and suppression systems. Smoke detectors, fire alarms, sprinkler systems, and fire extinguishers must be strategically placed throughout the facility and regularly tested to ensure they are in working order. The integration of these systems into the building’s design is not only a regulatory requirement but also a best practice in safeguarding human life.
Emergency preparedness extends beyond fire safety to encompass a range of potential disasters, including natural events like earthquakes and floods, as well as human-caused incidents such as chemical spills or acts of violence. Healthcare facilities must develop and regularly update their emergency operations plans (EOPs), which outline the procedures for responding to various emergencies. These plans should be tailored to the specific needs and capabilities of the facility and include clear communication protocols, resource allocation strategies, and roles and responsibilities for staff during an emergency.
Training is another essential element of emergency preparedness. Regular drills and exercises help familiarize staff with evacuation routes and procedures, the use of emergency equipment, and the execution of their roles within the EOP. Such training ensures that in the event of an actual emergency, everyone knows what to do and where to go, minimizing chaos and confusion.
Additionally, healthcare facilities must coordinate with local emergency services to ensure a seamless response in the event of a larger-scale disaster. This collaboration can include sharing of plans, joint training exercises, and establishing communication links that can be activated quickly when needed.
For healthcare administrators, maintaining up-to-date documentation is crucial for demonstrating compliance with TJC standards and other regulatory requirements related to fire safety and emergency preparedness. This includes records of system inspections, training sessions, drill outcomes, and any actual incidents that have occurred.
A robust approach to fire safety and emergency preparedness is a non-negotiable aspect of healthcare facility management. It requires ongoing attention to detail, investment in reliable safety systems, comprehensive planning, staff training, and collaboration with external agencies. By prioritizing these areas, healthcare facilities can provide a safer environment for all occupants and ensure that they are ready to respond effectively to any emergency situation that may arise.
Accessibility and Accommodation Provisions in Medical Buildings
Ensuring that healthcare facilities are accessible and accommodating to all patients, staff, and visitors is not just a matter of legal compliance—it is a fundamental aspect of providing compassionate and effective healthcare. Accessibility encompasses a broad range of considerations, from architectural design to the availability of assistive devices and services that support individuals with disabilities.
Healthcare buildings must comply with the Americans with Disabilities Act (ADA), which mandates that public spaces, including medical facilities, be accessible to individuals with a variety of disabilities. This includes providing ramps or lifts in place of stairs, installing automatic doors, ensuring that hallways and doorways are wide enough to accommodate wheelchairs, and equipping restrooms with appropriate fixtures such as grab bars and accessible toilets.
Beyond physical structures, accessibility also involves the provision of services such as sign language interpreters for the deaf or hard of hearing, materials in Braille for the visually impaired, and patient education resources in multiple languages or in formats accessible to those with learning disabilities. It is essential that these accommodations are thoughtfully integrated into the patient care strategy to ensure that all individuals receive equitable treatment and can navigate the healthcare system with dignity.
For individuals with mobility challenges, healthcare facilities must offer adequate parking spaces, drop-off zones, and seating arrangements. These features not only aid in accessibility but also contribute to the overall safety and comfort of patients as they move through the facility. Additionally, adjustable examination tables and imaging equipment are necessary to provide safe and comfortable care to patients regardless of their physical abilities.
Administrators and facility managers must regularly assess their buildings and services to identify areas where accessibility can be improved. This may involve consulting with disability advocates, conducting surveys with patients and staff, or reviewing incident reports for patterns that indicate accessibility issues. By proactively addressing these concerns, healthcare facilities can create an inclusive environment that caters to the needs of all individuals.
Maintaining compliance with TJC standards and other regulatory requirements is an ongoing process that involves regular training for staff on how to assist patients with disabilities effectively. Staff should be familiar with the use of assistive technologies, understand how to navigate accessibility features within the facility, and be prepared to respond to the unique needs of patients with compassion and competence.
Ultimately, the goal is to create a healthcare setting that empowers all individuals to access care without barriers. This commitment to accessibility and accommodation not only fulfills legal obligations but also reflects the healthcare industry’s dedication to providing high-quality care to every member of the community.
Ongoing Compliance: Inspections, Maintenance, and Documentation
Maintaining ongoing compliance with TJC regulations and other healthcare standards is a dynamic and continuous process that requires diligent attention to inspections, maintenance, and documentation. Regular inspections are a cornerstone of this process, ensuring that all aspects of the healthcare facility—from the physical environment to the equipment used—are in line with current regulatory requirements. These inspections can be internal or conducted by external bodies, and they serve as a critical check to identify areas that may need improvement or pose potential risks to patient safety.
Effective maintenance programs are equally important in sustaining a safe healthcare environment. This includes routine checks and servicing of medical equipment, emergency generators, HVAC systems, and fire safety equipment. Preventive maintenance not only extends the lifespan of critical infrastructure but also minimizes the risk of sudden failures that could compromise patient care or safety. Healthcare facilities must have a systematic approach to maintenance, with schedules that are strictly adhered to and documented.
Documentation plays a pivotal role in ongoing compliance. It provides a clear record of all actions taken to maintain standards and is essential for demonstrating compliance during TJC surveys or audits by other regulatory agencies. Documentation should be thorough, organized, and easily retrievable. It must include details of inspections, maintenance activities, staff training sessions, policy updates, and any incidents or corrective actions taken in response to deficiencies.
Healthcare leaders must ensure that their staff are well-trained in compliance protocols and understand the importance of their roles in maintaining a compliant facility. This includes providing ongoing education on the latest TJC standards, changes in federal or state regulations, and best practices in healthcare safety and quality. Staff should be encouraged to report potential compliance issues promptly and be assured that such reports will be addressed seriously and constructively.
Technology can be leveraged to streamline the compliance process. Digital systems for tracking maintenance, electronic health records for documenting patient care, and online platforms for staff training can enhance efficiency and accuracy. However, it is crucial that these systems are secure and compliant with patient privacy laws such as HIPAA.
Ultimately, the goal of ongoing compliance is to foster a culture of safety and quality within the healthcare facility. It is not just about passing inspections or avoiding penalties; it is about consistently providing a safe and healing environment for patients. Executives, administrators, managers, and safety coordinators must work collaboratively to integrate compliance into the daily operations of their facilities, ensuring that it becomes a natural part of the organizational ethos.
By prioritizing inspections, maintenance, and documentation, healthcare facilities can uphold the high standards set by TJC and other regulatory bodies. This commitment to excellence not only safeguards the well-being of patients but also enhances the reputation of the facility as a trusted provider of quality healthcare services.

“Ensuring Safe and Sustainable Healthcare Facilities: Your Ultimate Building Code Compliance FAQ Guide”
Frequently Asked Questions about Building Code Compliance for Healthcare Facilities
Understanding the building codes and their implications for life safety in healthcare environments is crucial for ensuring the well-being of patients, staff, and visitors. Below are answers to some common questions related to building code compliance in healthcare facilities:
-
Why is building code compliance important for healthcare facilities?
Building code compliance is vital for healthcare facilities as it helps ensure the safety and security of everyone within the facility. By adhering to these codes, healthcare environments can minimize the risk of fires, structural failures, and other hazards. Compliance also helps healthcare facilities meet legal requirements and maintain accreditation.
-
What are some key building code requirements for healthcare facilities?
Some key building code requirements for healthcare facilities include adequate means of egress, fire-resistant construction materials, proper ventilation systems, accessible entrances and exits, appropriate electrical systems, and emergency lighting. These requirements aim to enhance life safety and provide a secure environment for patients, staff, and visitors.
-
How can healthcare facilities ensure compliance with building codes?
To ensure compliance with building codes, healthcare facilities should engage the services of qualified architects, engineers, and consultants who specialize in healthcare facility design. These professionals have a deep understanding of the codes and can guide the facility through the design, construction, and renovation processes while ensuring compliance at every step.
-
What happens if a healthcare facility fails to comply with building codes?
If a healthcare facility fails to comply with building codes, it may face serious consequences. These can include fines, legal liabilities in case of accidents or injuries, loss of accreditation or certification, and even closure of the facility. Non-compliance not only jeopardizes the safety of occupants but also damages the reputation and trust of the healthcare organization.
-
Are there any resources available to assist healthcare facilities in understanding building codes?
Absolutely! Many resources are available to assist healthcare facilities in understanding building codes. Building code handbooks, online databases, and industry associations provide valuable information and guidance. Additionally, consulting with experienced professionals in healthcare facility design and code compliance can offer practical solutions tailored to the specific needs of the facility.
By staying informed about building code compliance and actively working towards meeting these requirements, healthcare facilities can create a safe and secure environment that promotes the well-being of all individuals within their care.

